Total Knee Replacement
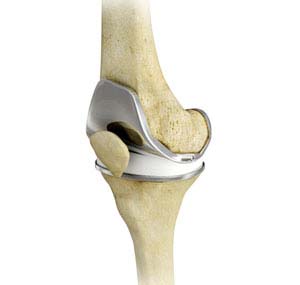
Knee arthritis is a common condition, which is initially managed with nonoperative or non-surgical treatment options. These often give people improvement initially, but over time arthritis progresses and eventually for many patients, these will become less effective. Eventually many patients come to a point where they request surgery to help with their pain. This is different for every patient. Arthritis progresses differently for patients, and different patients have different activity levels and daily or work requirements, which will affect people in different ways. When to undergo surgery is a discussion to have with your doctor, and ultimately the decision comes down to you, the patient. Surgery for knee arthritis is an elective surgery, it is not required. It is a decision you as a patient have to be ready for because every surgery will have risks that have to be outweighed by the benefits, and you have to be at a point where you are willing to accept those risks because the benefit of surgery and improvement in pain and function are worth it. You also will have rehabilitation that goes along with this, and it will take months of work from you as a patient, where as it will only take hours of work from me as your doctor. You have to be ready to put in the work, because you will get out of this what you put into it. A perfectly executed surgery will ultimately have inferior results if appropriate rehab is not performed. And this requires involvement from you as a patient. The best therapist around canʼt do it for you.
Once you have reached the point (physically, mentally, and emotionally) where you are ready to proceed with surgery and the accompanying rehab, surgery for the vast majority of patients comes down to resurfacing or replacement (also called arthroplasty). For the majority of patients dealing with knee arthritis, a total knee replacement is the best choice. Only 10-15% of patients are felt to be candidates for partial knee replacements. A total knee replacement is a very good surgery for knee arthritis that has failed appropriate non-operative treatment options. It is highly successful at improving and potentially even eliminating pain, and improves function. It however is a major surgery, and with this comes risks and trade-offs. While literally thousands of people every month are satisfied and pleased with their outcomes after a knee replacement, there are some that are not. And that is something everyone needs to understand and accept before signing up for surgery.
Total knee replacements have risks like all surgeries, such as pain, scarring, potential damage to nearby structures, and anesthetic related risks, which are overall fairly rare in healthy individuals. A devastating complication after a total joint replacement is infection. While this also happens infrequently (~1-2% in healthy individuals), if this complication happens it cannot be treated with antibiotics alone. It requires more surgery to clean out the joint and exchange parts. Sometimes the entire prosthesis has to be removed and replaced with an antibiotic spacer. This is a long and arduous process that no one wants to go through. The risks are higher in certain populations, like diabetics, patients who are obese, smokers, patients with inflammatory arthropathies or auto-immune disease. This all needs to be weighed and considered before surgery. Any modifiable risk factors should be addressed and corrected to help lower your risk as much as possible (for example obtaining better glucose control for diabetics, stopping smoking, or losing weight).
Other potential complications are stiffness (which sometimes can require a manipulation under anesthesia), weakness, loss of function or difficulty with certain activities. Knees tend to lose motion as arthritis progresses. Stiffness is a major concern which can impact daily functional activities, both before and after surgery. The amount of motion you have after your knee replacement is directly related to the amount of motion you have prior to your surgery. Knees that are stiff before surgery will be stiff after surgery. This can be a difficult problem to address, and appropriate expectations before surgery is the best way to address this problem! Difficulty kneeling on the affected knee and deep squats after a knee replacement are common complaints for many patients. It doesnʼt affect the implants, but can range from discomfort to down right painful for patients. And this can be permanent. Another common problem is numbness on the lateral (or outside) aspect of the knee and just below over the outside portion of the upper calf. This is from a nerve that crosses the area of the incision which is often cut. It is expected and nothing to be concerned about, but is also often permanent.
A recent concern after knee replacement is difficulty with how a patient perceives the knee, or feeling like it isnʼt normal (the patient is not satisfied with their outcome)1. This is something I think is becoming more apparent for several reasons: knee replacements are performed on younger and more active patients, older patients are staying active longer, we put less restrictions of patients after knee replacements, and honestly simply the fact that we are now asking how the patient feels the knee works after surgery as a measure of successful outcome, rather than simply what the x-ray looks like or how long the knee replacement lasts. This topic is under the magnifying glass currently, with a lot of interest and research under way to try to improve this. Some studies would suggest that as many as 40% of patients can be unhappy with their knee replacement. Not to say that knee replacement isnʼt successful at eliminating the debilitating pain of arthritis and improving function, but we should always remember that it is a replacement, not a normal knee.
As we strive to more accurately reproduce the way the knee works, things like robotic assisted surgery (for example Mako robotic-arm assisted surgery) have gained favor in hopes of more accurately placing and balancing knee replacements. While we do not have long term data yet, numerous studies have shown earlier rehabilatation goals and less swelling when compared to manual or conventional knee replacements3. I personally feel that over time these will help us achieve a more accurate knee replacement which will help patients feel closer to normal as they maintain their active lifestyle. Early experience with this technology has certainly been exciting and promising.
- Patient Satisfaction after Total Knee Arthroplasty: Who is Satisfied and Who is Not? Bourne, R.B., Chesworth, B.M., Davis, A.M. et al. Clin Orthop Relat Res (2010) 468: 57.
- Patient dissatisfaction following total knee replacement A GROWING CONCERN? D. Nam, R. M. Nunley, R. L. Barrack. Bone Joint J 2014;96-B(11 Suppl A):96–100.
- Robotic-arm assisted total knee arthroplasty is associated with improved early functional recovery and reduced time to hospital discharge compared with conventional jig-based total knee arthroplasty A PROSPECTIVE COHORT STUDY. B. Kayani, S. Konan, J. Tahmassebi, J. R. T. Pietrzak, F. S. Haddad. Bone and Joint Journal: 2018; 100-B:930–7.







